Life Expectancy
Across the world, people are living longer.
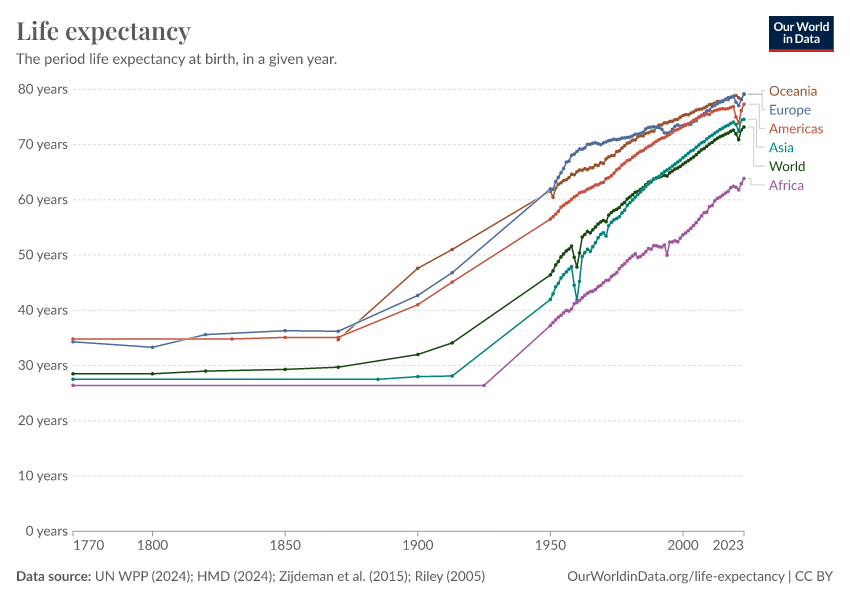
In 1900, the average life expectancy of a newborn was 32 years. By 2021 this had more than doubled to 71 years.
But where, when, how, and why has this dramatic change occurred?
To understand it, we can look at data on life expectancy worldwide.
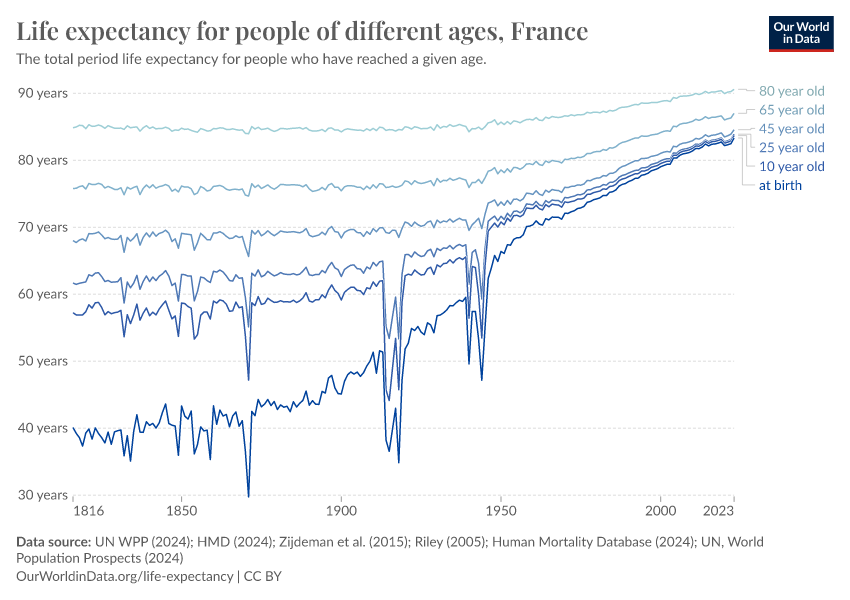
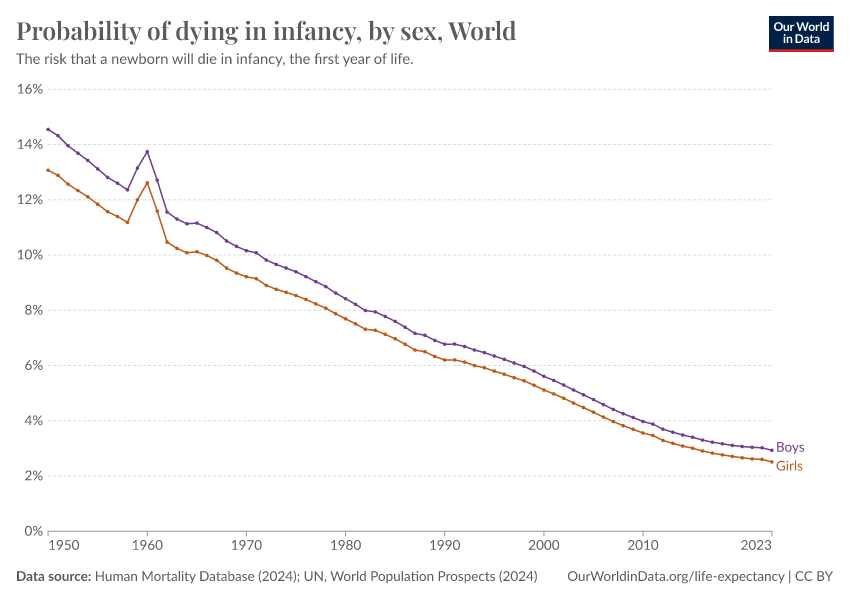
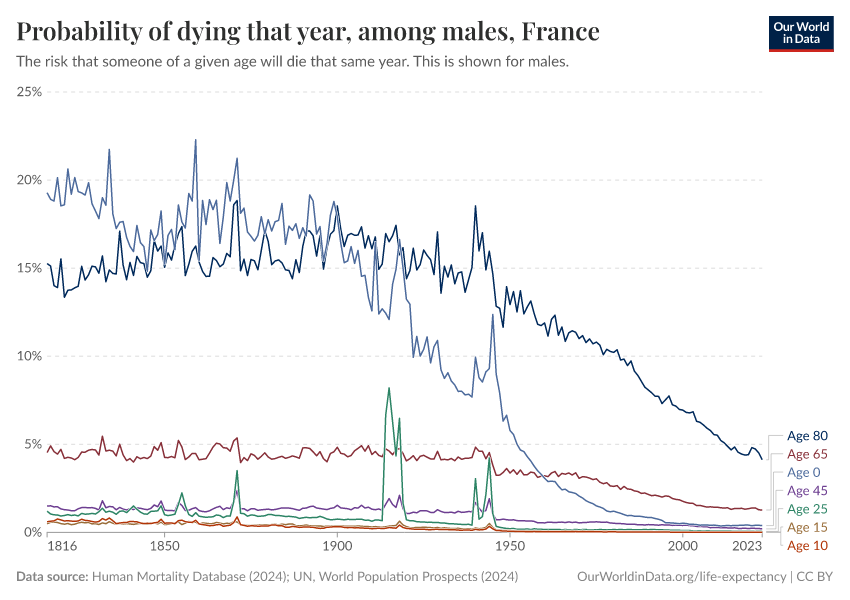
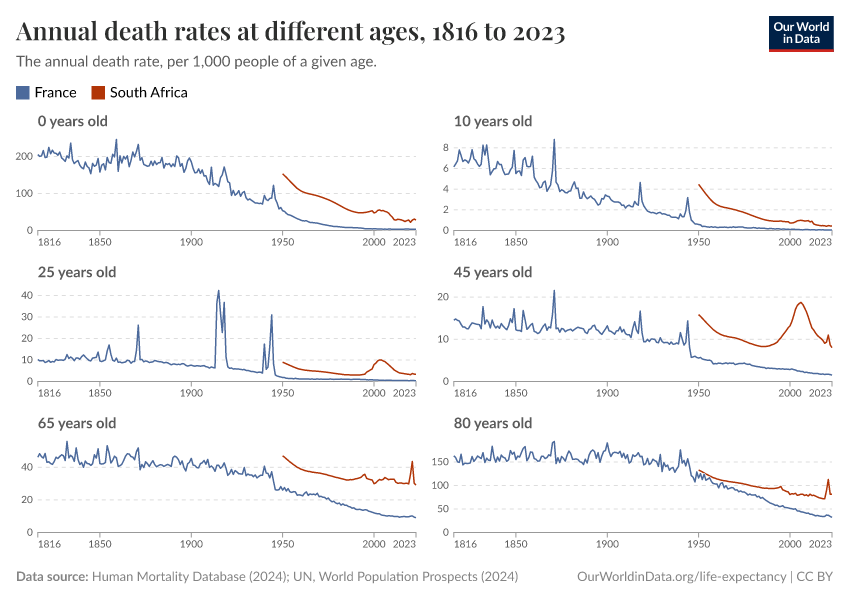
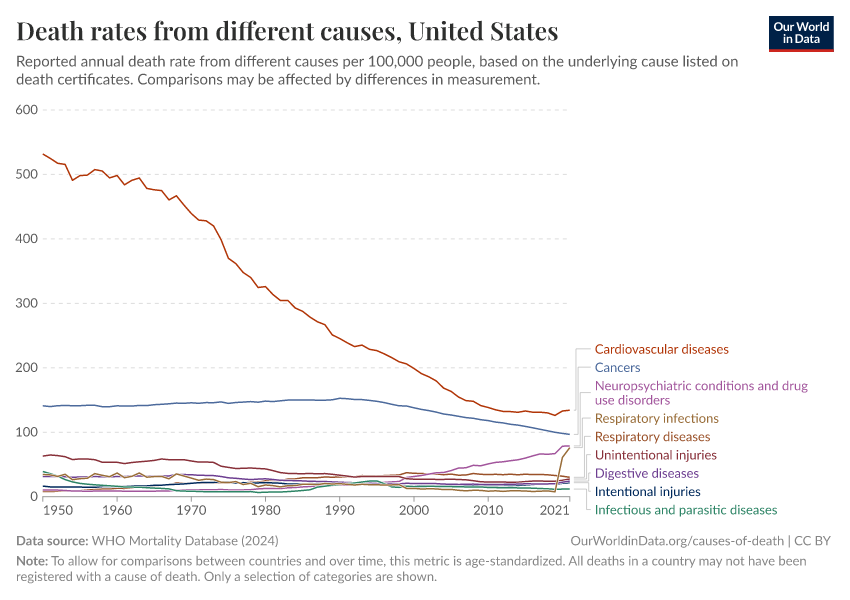
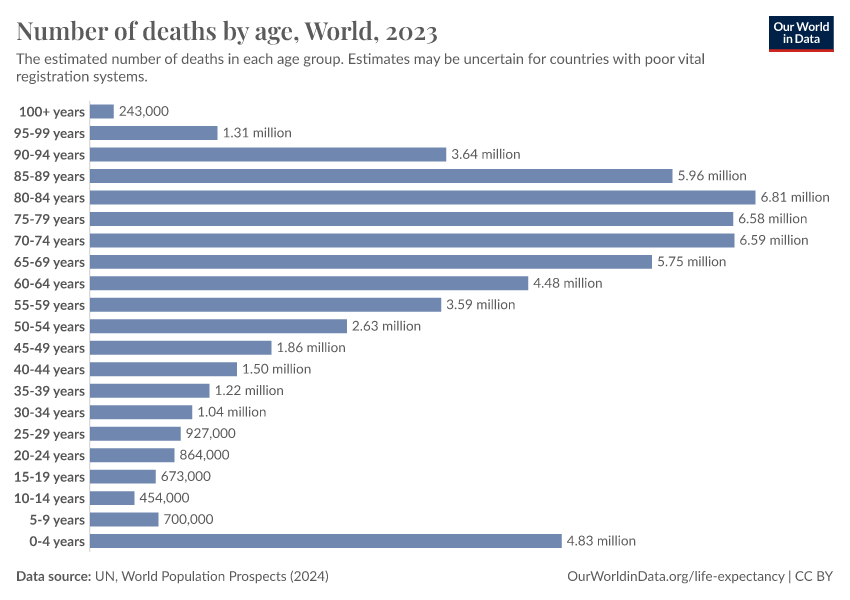
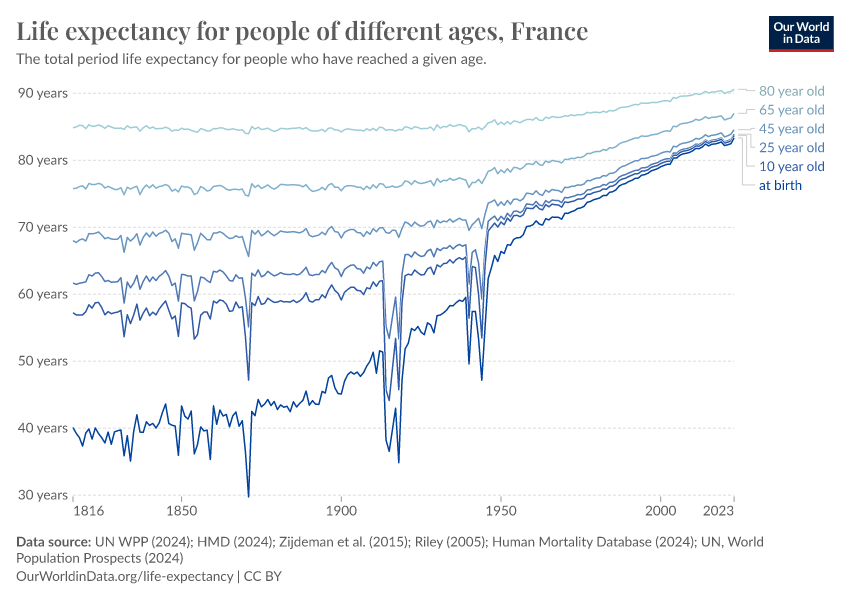
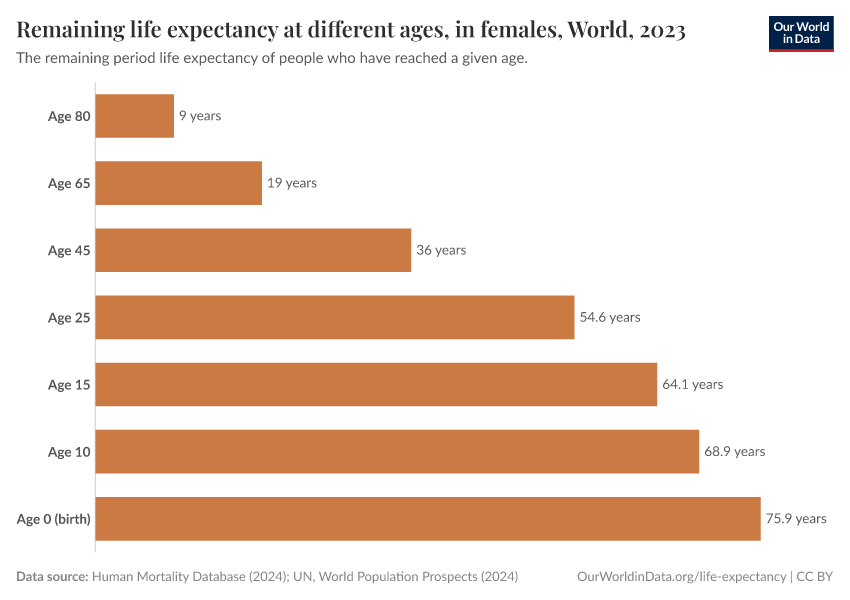
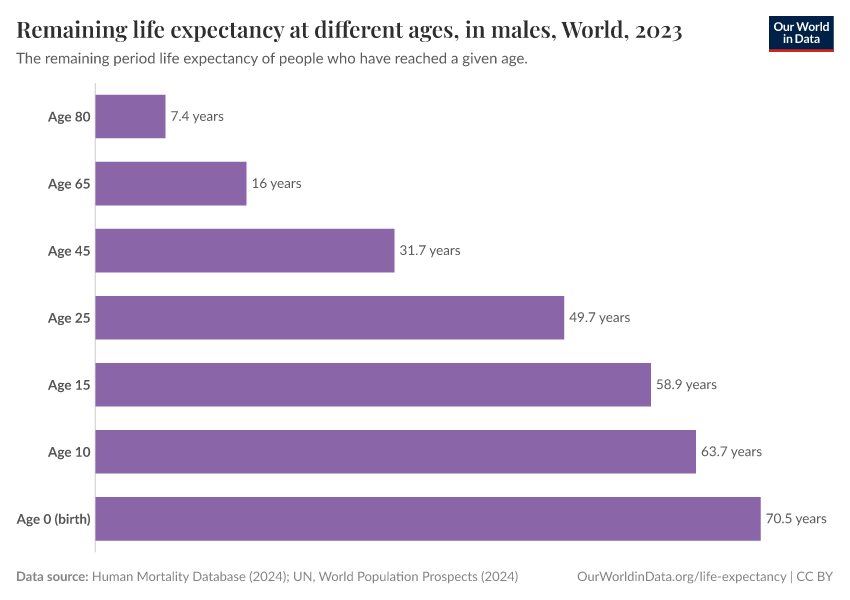
The large reduction in child mortality has played an important role in increasing life expectancy. But life expectancy has increased at all ages. Infants, children, adults, and the elderly are all less likely to die than in the past, and death is being delayed.
This remarkable shift results from advances in medicine, public health, and living standards. Along with it, many predictions of the ‘limit’ of life expectancy have been broken.
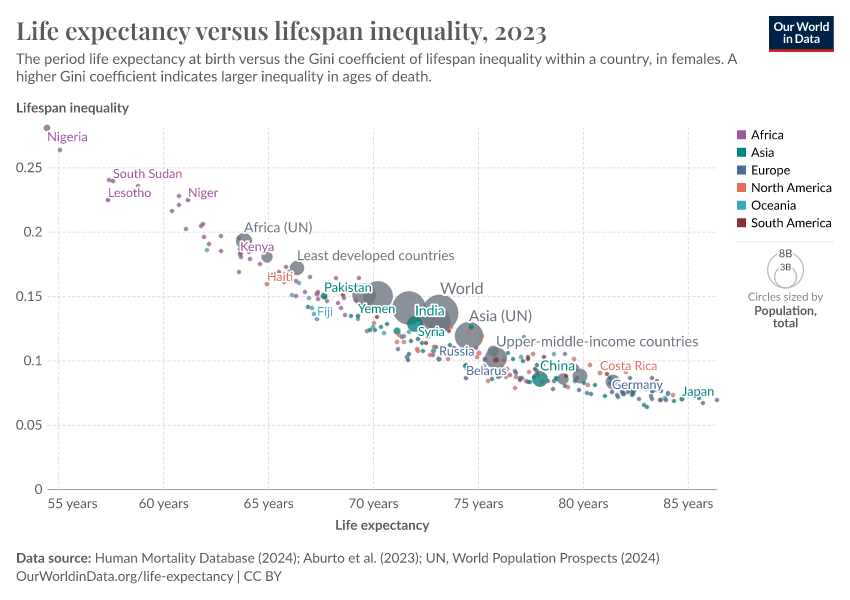
On this page, you will find global data and research on life expectancy and related measures of longevity: the probability of death at a given age, the sex gap in life expectancy, lifespan inequality within countries, and more.
Research & Writing
More articles on life expectancy
August 28, 2017
Life expectancy: what does this actually mean?
March 1, 2020
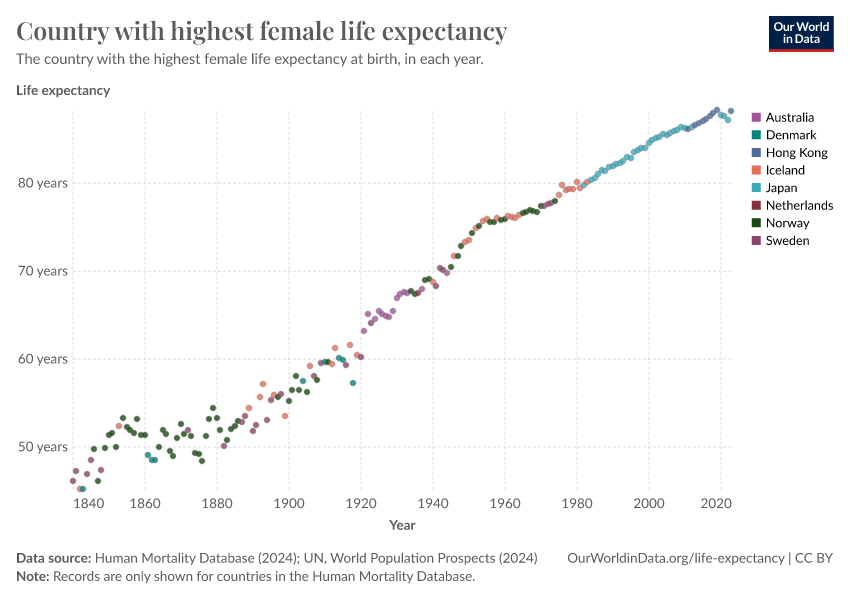
The rise of maximum life expectancy
November 27, 2023
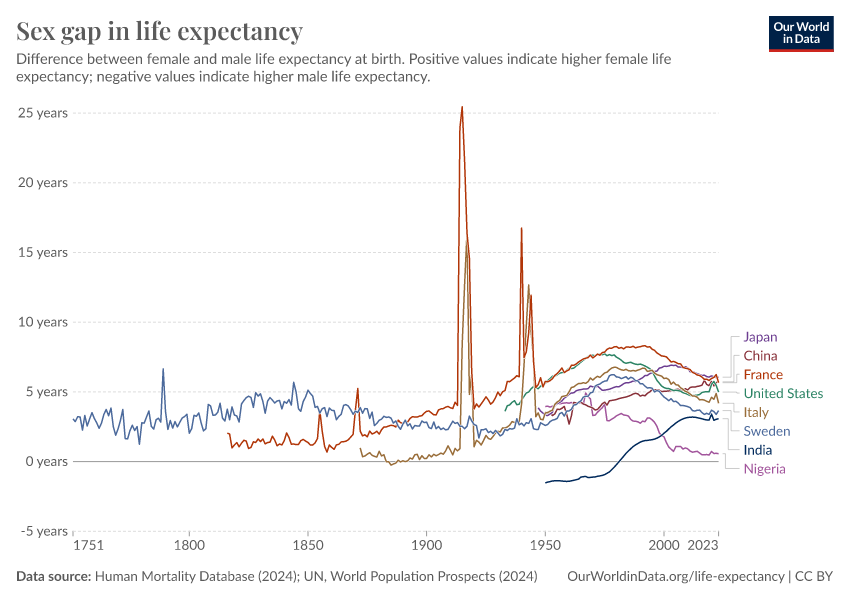
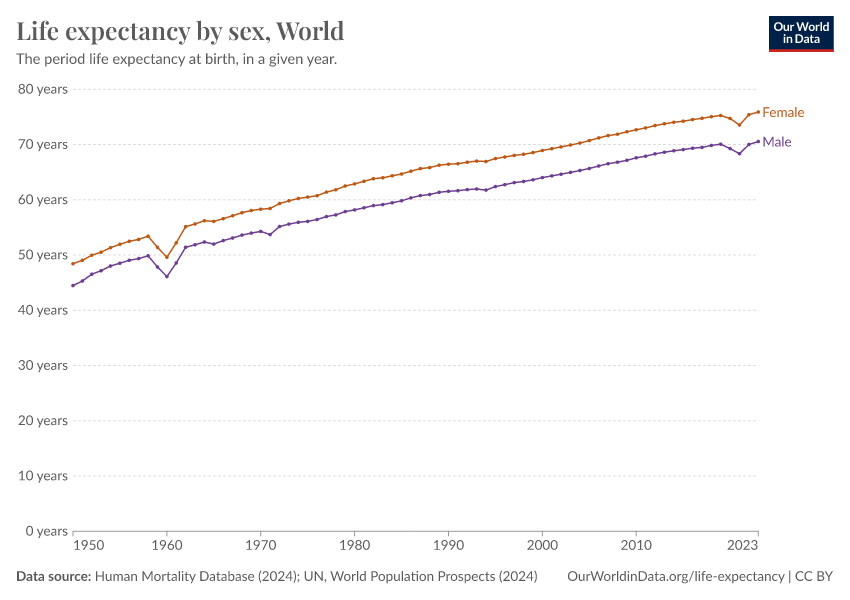
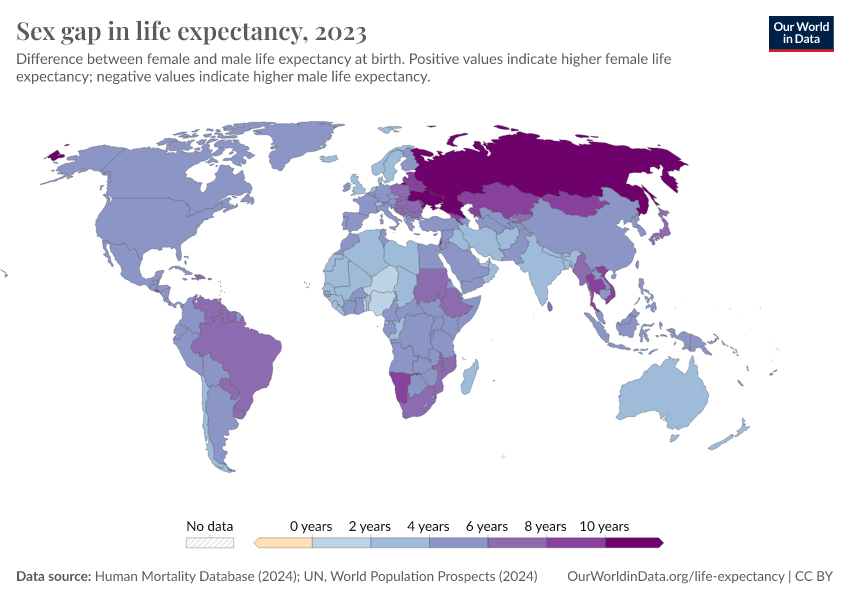
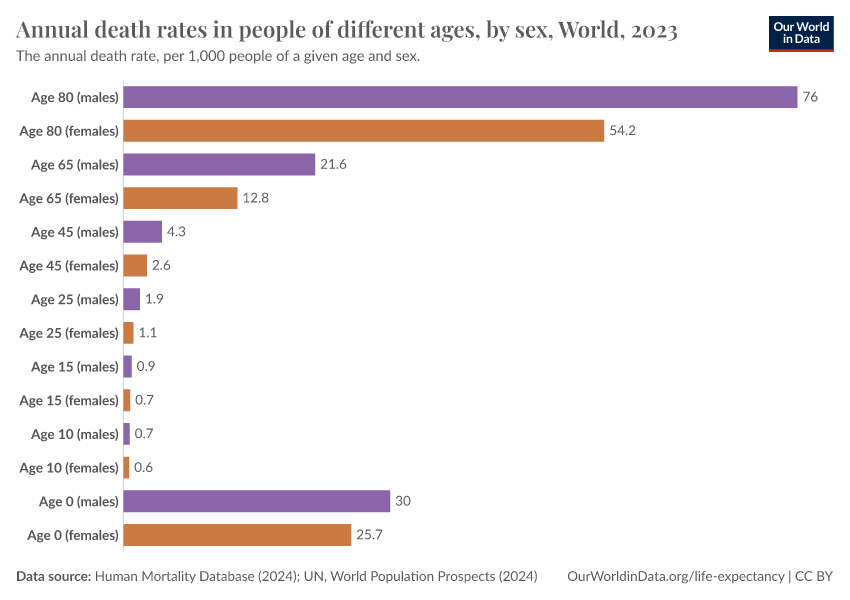
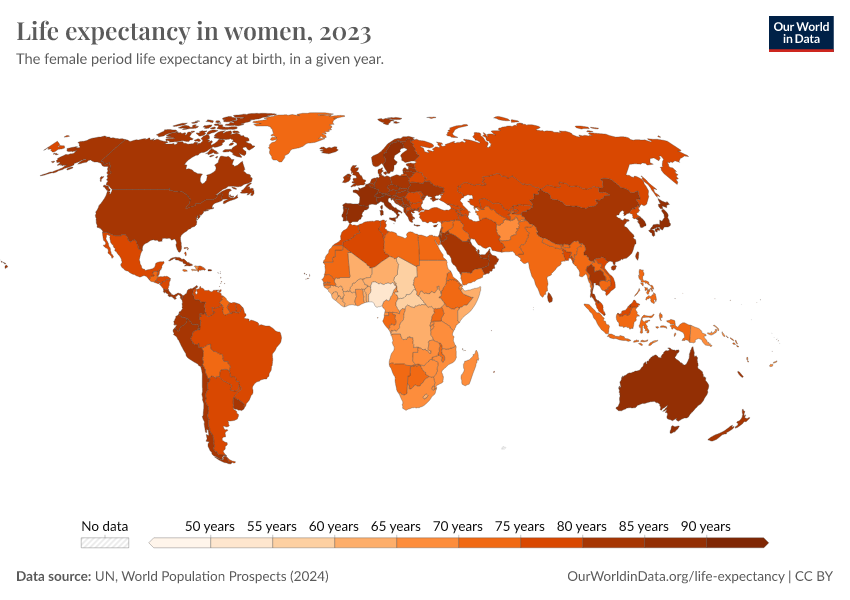
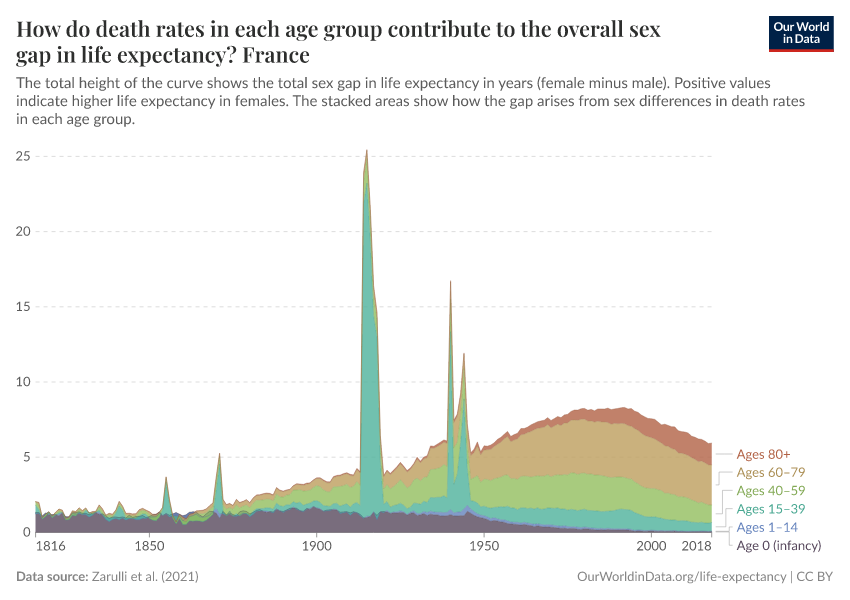
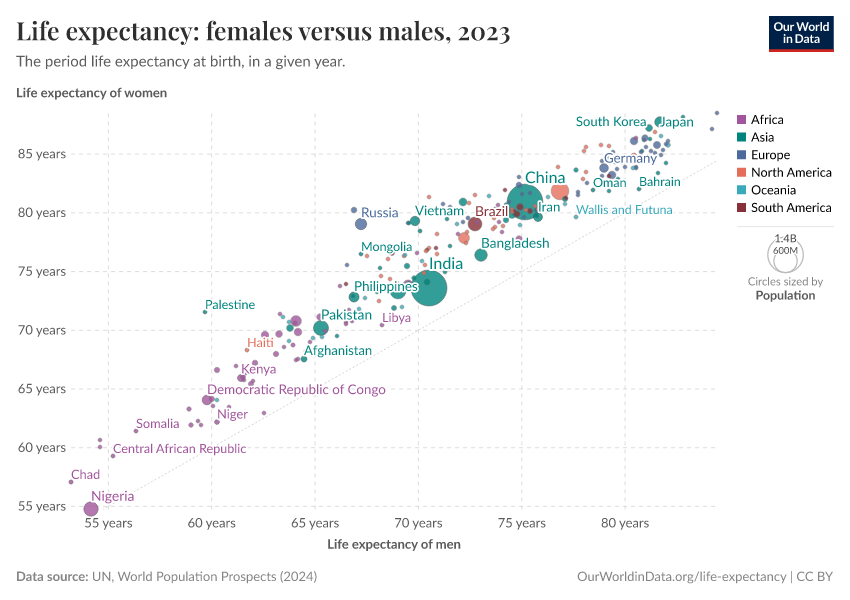
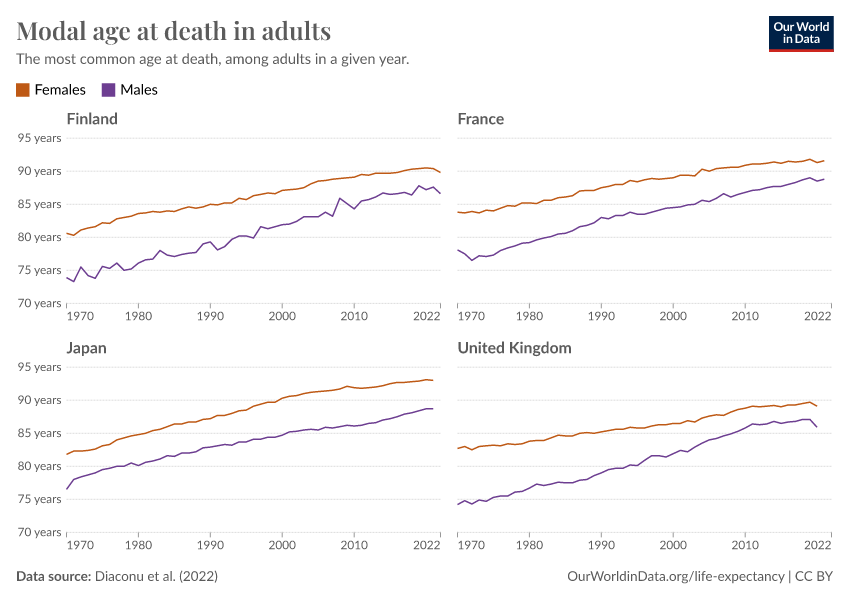
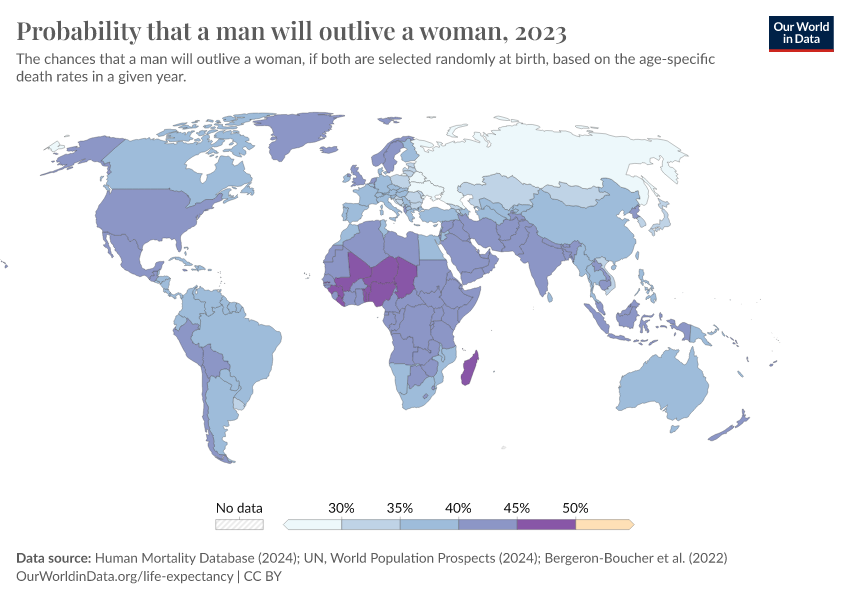
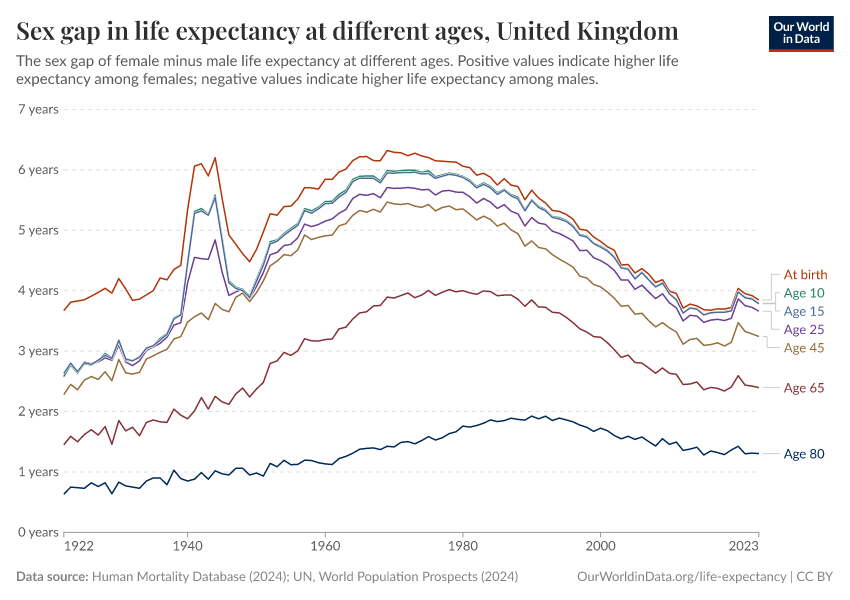
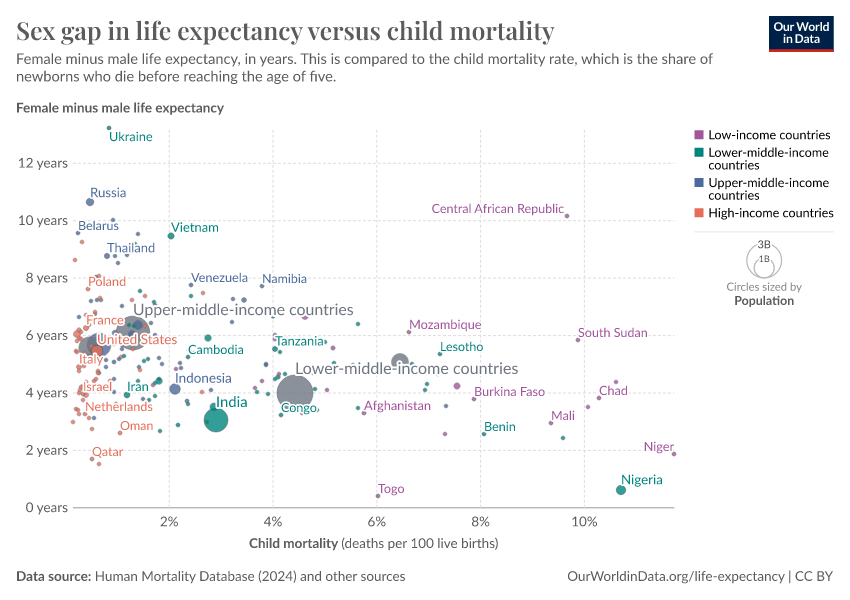
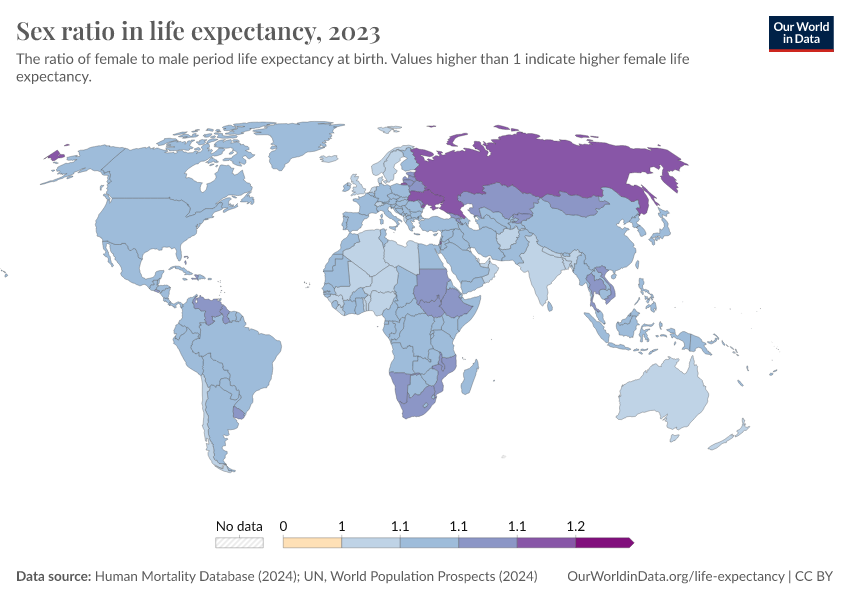
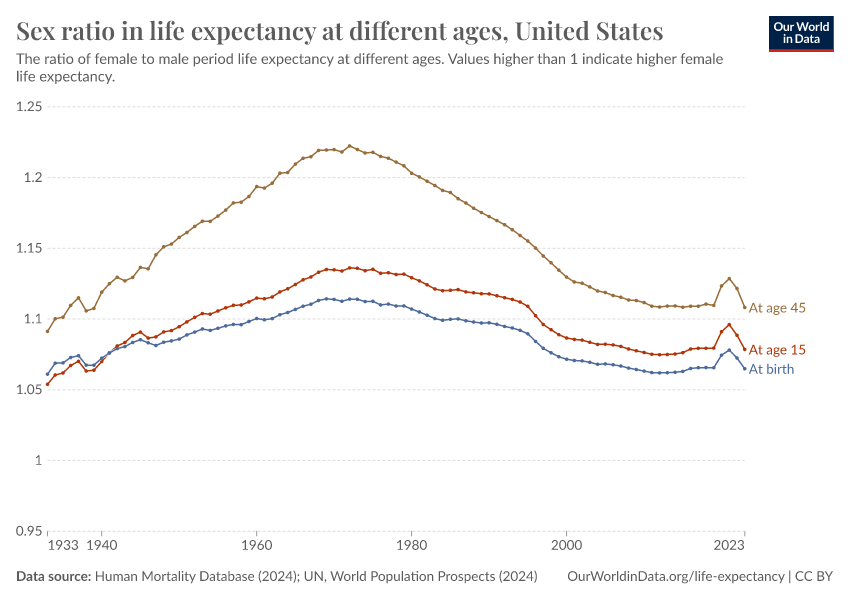
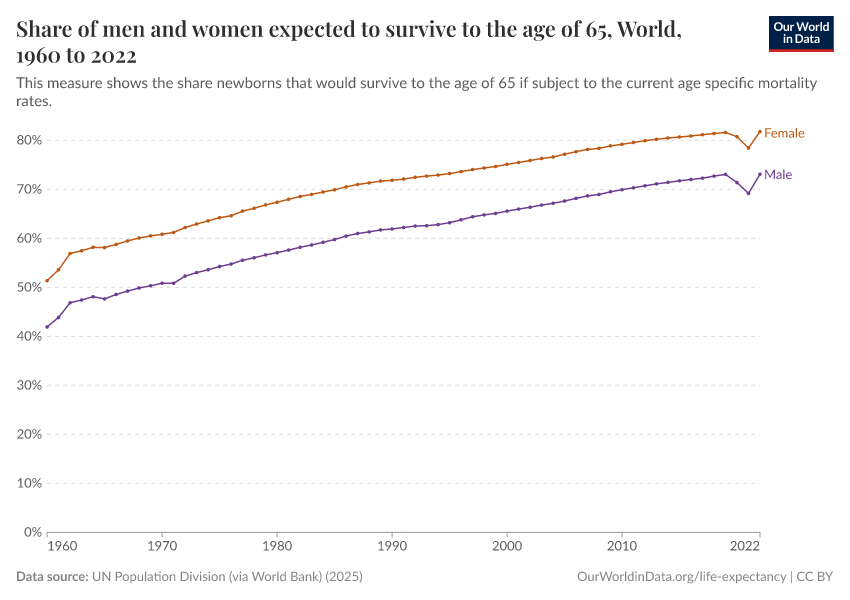
Why do women live longer than men?
October 13, 2023
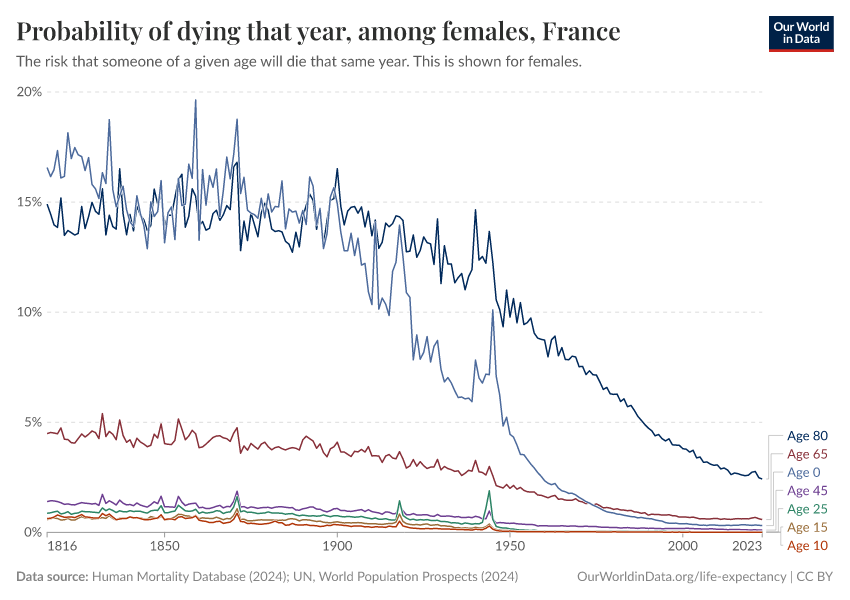
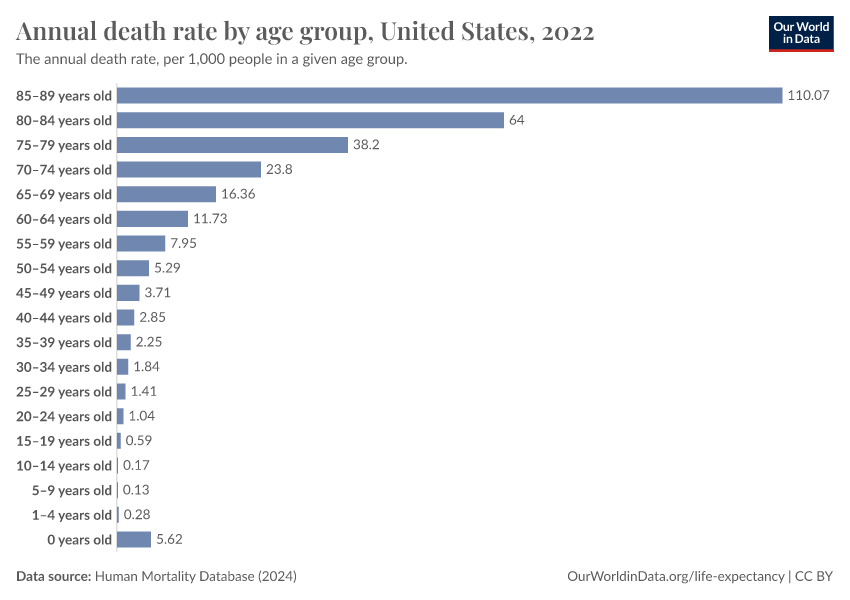
How does the risk of death change as we age – and how has this changed over time?
November 27, 2023
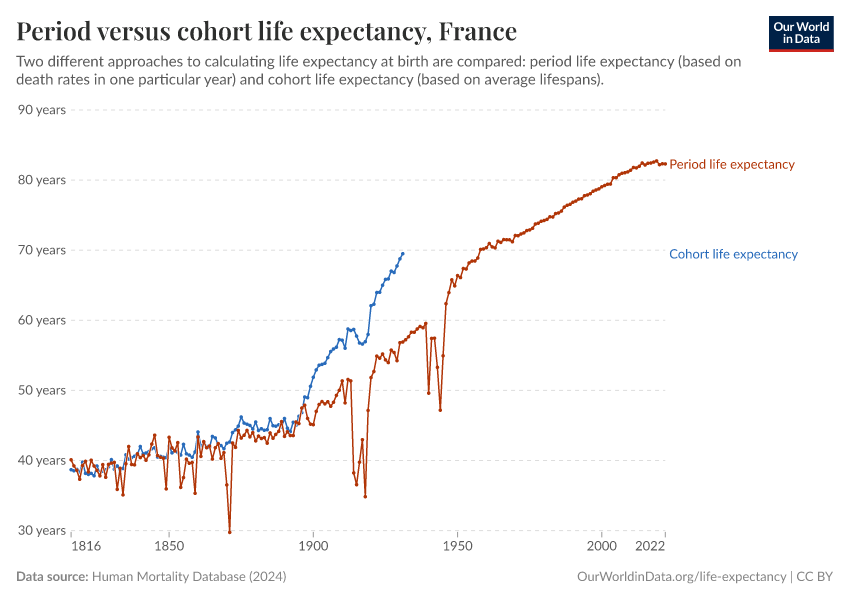
Period versus cohort measures: what’s the difference?
September 23, 2020
It’s not just about child mortality; life expectancy increased at all ages
March 4, 2020
The Spanish flu: the global impact of the largest influenza pandemic in history
October 29, 2020
Why is life expectancy in the US lower than in other rich countries?
Key Charts on Life Expectancy
See all charts on this topicFeatured Data on Life Expectancy
Endnotes
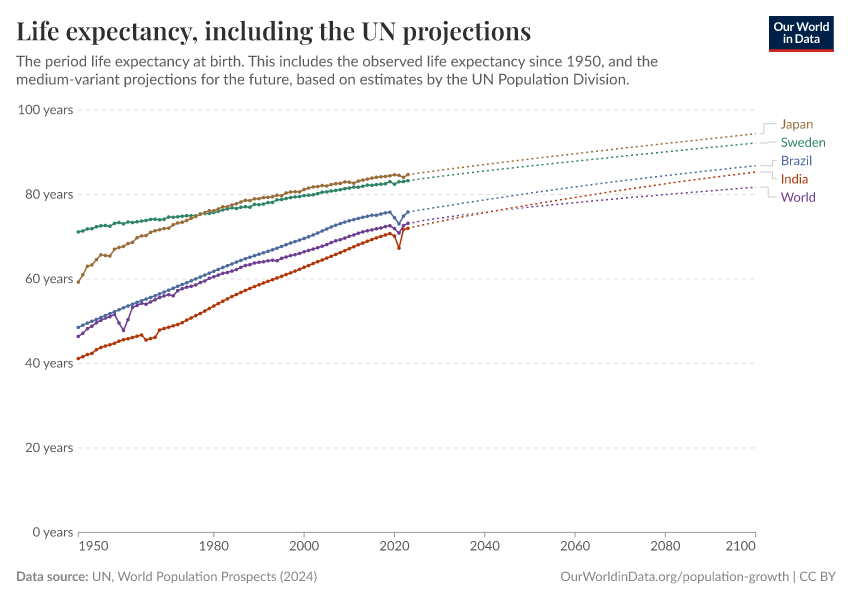
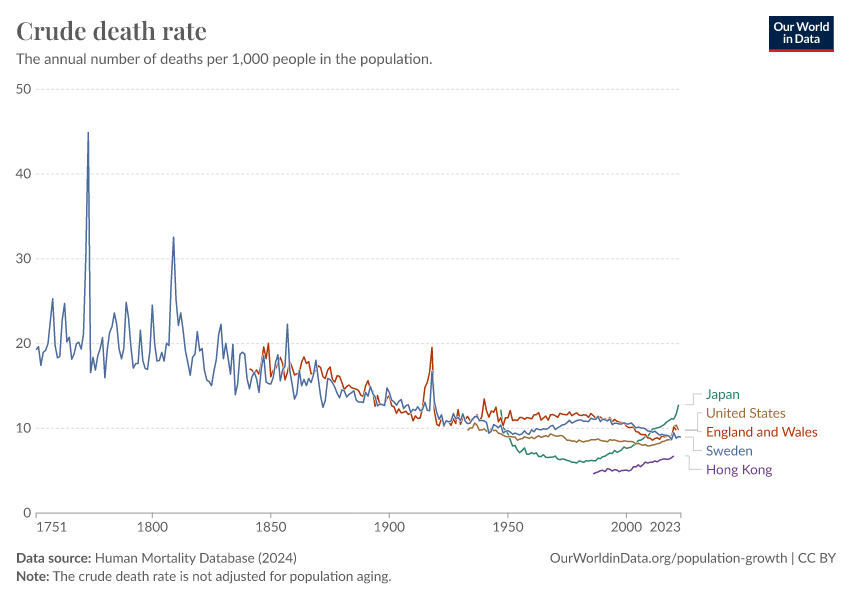
As you can see, the chart also shows that the rise has not been completely constant. Major events – the World Wars, the 1918 Spanish flu pandemic, the HIV/AIDS epidemic, and the COVID-19 pandemic – have had a major impact on mortality rates and left a visible mark on life expectancy.
Zijdeman, Richard and Filipa Ribeira da Silva (2015). Life Expectancy at Birth (Total). http://hdl.handle.net/10622/LKYT53 , accessed via the Clio Infra website. Zijdeman, R. L., & de Silva, F. R. (2014). Life expectancy since 1820.
Riley, J. C. (2005). Estimates of regional and global life expectancy, 1800–2001. Population and Development Review, 31(3), 537–543.
Barbieri, M., Wilmoth, J. R., Shkolnikov, V. M., Glei, D., Jasilionis, D., Jdanov, D., Boe, C., Riffe, T., Grigoriev, P., & Winant, C. (2015). Data Resource Profile: The Human Mortality Database (HMD). International Journal of Epidemiology, 44(5), 1549–1556. https://doi.org/10.1093/ije/dyv105
Wrigley E.A. et al. (1997) English population history from family reconstitution 1580-1837, Cambridge University Press, Cambridge.
Kannisto, V., Nieminen, M. and O. Turpeinen (1999), “Finnish life tables since 1751,” Demographic Research, Vol. 1/1.
Aburto, J. M., Villavicencio, F., Basellini, U., Kjærgaard, S., & Vaupel, J. W. (2020). Dynamics of life expectancy and life span equality. Proceedings of the National Academy of Sciences, 117(10), 5250–5259. https://doi.org/10.1073/pnas.1915884117
Liou, L., Joe, W., Kumar, A., & Subramanian, S. V. (2020). Inequalities in life expectancy: An analysis of 201 countries, 1950–2015. Social Science & Medicine, 253, 112964. https://doi.org/10.1016/j.socscimed.2020.112964
Permanyer, I., & Scholl, N. (2019). Global trends in lifespan inequality: 1950-2015. PLOS ONE, 14(5), e0215742. https://doi.org/10.1371/journal.pone.0215742
Vaupel, J. W., Zhang, Z., & Van Raalte, A. A. (2011). Life expectancy and disparity: An international comparison of life table data. BMJ Open, 1(1), e000128–e000128. https://doi.org/10.1136/bmjopen-2011-000128
Wilson, C. (2011). Understanding Global Demographic Convergence since 1950. Population and Development Review, 37(2), 375–388. https://doi.org/10.1111/j.1728-4457.2011.00415.x
Aburto, J. M., Villavicencio, F., Basellini, U., Kjærgaard, S., & Vaupel, J. W. (2020). Dynamics of life expectancy and life span equality. Proceedings of the National Academy of Sciences, 117(10), 5250–5259. https://doi.org/10.1073/pnas.1915884117
Zarulli, V., Kashnitsky, I., & Vaupel, J. W. (2021). Death rates at specific life stages mold the sex gap in life expectancy. Proceedings of the National Academy of Sciences, 118(20), e2010588118. https://doi.org/10.1073/pnas.2010588118
Vladimir Canudas-Romo, Nandita Saikia, & Nadia Diamond-Smith. (2016). The contribution of age-specific mortality towards male and female life expectancy differentials in India and selected States, 1970-2013. Asia-Pacific Population Journal, 30(2), 1–20. https://doi.org/10.18356/8ec0129d-en
Drevenstedt, G. L., Crimmins, E. M., Vasunilashorn, S., & Finch, C. E. (2008). The rise and fall of excess male infant mortality. Proceedings of the National Academy of Sciences, 105(13), 5016–5021. https://doi.org/10.1073/pnas.0800221105
Feraldi, A., & Zarulli, V. (2022). Patterns in age and cause of death contribution to the sex gap in life expectancy: A comparison among ten countries. Genus, 78(1), 23. https://doi.org/10.1186/s41118-022-00171-9
Janssen, F. (2020). Changing contribution of smoking to the sex differences in life expectancy in Europe, 1950–2014. European Journal of Epidemiology, 35(9), 835–841. https://doi.org/10.1007/s10654-020-00602-x
Luy, M., & Wegner-Siegmundt, C. (2015). The impact of smoking on gender differences in life expectancy: More heterogeneous than often stated. The European Journal of Public Health, 25(4), 706–710. https://doi.org/10.1093/eurpub/cku211
Glei, D. A., & Horiuchi, S. (2007). The narrowing sex differential in life expectancy in high-income populations: Effects of differences in the age pattern of mortality. Population Studies, 61(2), 141–159. https://doi.org/10.1080/00324720701331433
Bergeron-Boucher, M.-P., Alvarez, J.-A., Kashnitsky, I., & Zarulli, V. (2022). Probability of males to outlive females: An international comparison from 1751 to 2020. BMJ Open, 12(8), e059964. https://doi.org/10.1136/bmjopen-2021-059964
Oeppen, J., & Vaupel, J. W. (2002). Broken Limits to Life Expectancy. Science, 296(5570), 1029–1031. https://doi.org/10.1126/science.1069675
Dublin, L., Israel. (1928). Health and Wealth: A Survey of the Economics of World Health. Harper & Brothers.
Cite this work
Our articles and data visualizations rely on work from many different people and organizations. When citing this topic page, please also cite the underlying data sources. This topic page can be cited as:
Saloni Dattani, Lucas Rodés-Guirao, Hannah Ritchie, Esteban Ortiz-Ospina, and Max Roser (2023) - “Life Expectancy” Published online at OurWorldinData.org. Retrieved from: 'https://ourworldindata.org/life-expectancy' [Online Resource]BibTeX citation
@article{owid-life-expectancy,
author = {Saloni Dattani and Lucas Rodés-Guirao and Hannah Ritchie and Esteban Ortiz-Ospina and Max Roser},
title = {Life Expectancy},
journal = {Our World in Data},
year = {2023},
note = {https://ourworldindata.org/life-expectancy}
}Reuse this work freely
All visualizations, data, and articles produced by Our World in Data are completely open access under the Creative Commons BY license. You have the permission to use, distribute, and reproduce these in any medium, provided the source and authors are credited.
The data produced by third parties and made available by Our World in Data is subject to the license terms from the original third-party authors. We will always indicate the original source of the data in our documentation, so you should always check the license of any such third-party data before use and redistribution.
All of our charts can be embedded in any site.