Why do women live longer than men?
Women tend to live longer than men in all countries — but the sex gap in life expectancy is not a constant.
Women tend to live longer than men. In 2021, this difference amounted to a 5-year gap in global life expectancy: the average life expectancy was 73.8 years for women versus 68.4 years for men.
What causes these differences? Is it because women outlive men at old ages? Or because young men are more likely to experience accidents and violent deaths?
In this article, we’ll examine the sex gap in life expectancy: how it arises, how it varies around the world, and how it has shifted over generations.
The sex gap in life expectancy is not a constant
Women tend to outlive men around the world.
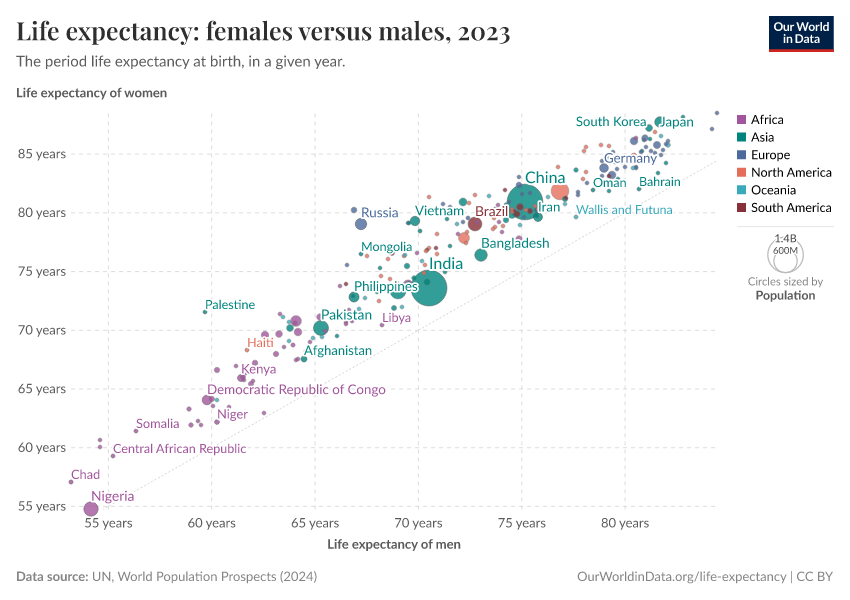
The chart below shows the difference. It compares female and male life expectancy across countries. Male life expectancy is shown on the horizontal axis, and female life expectancy is shown on the vertical axis.
All countries lie above the diagonal line, meaning female life expectancy is higher.
But the chart also shows that the gap varies between countries: some are much further from the line than others.
This is also visible in the map below. In some countries, like Russia, Belarus, and Ukraine, the gap is large — more than 10 years in 2021.
In other countries, such as Nigeria, it is less than 2 years.1
The next chart shows how the sex gap has changed over time.
Large spikes are visible during major wars, reflecting the fact that many young men died then.
You can also see that the gap gradually widened in many countries over the 20th century but has narrowed again in recent decades.
These charts show that the sex gap in life expectancy is not a constant. It varies between countries and has changed over time.
But why does this happen? And where does this gap come from?
A refresher on period life expectancy and what it means
Before we dive into the reasons for the sex gap in life expectancy, let’s consider how life expectancy is measured.
In this article, the data refers to the period life expectancy, a metric that summarizes death rates across all age groups in one particular year.
For a given year, it represents the average lifespan for a hypothetical group of people, if they experienced the same age-specific death rates throughout their whole lives as the age-specific death rates seen in that particular year.
This means it is directly influenced by factors that affect death rates, such as changes in living standards, public health and medicine, behaviors, and events like wars and pandemics.
You can read more about this here:
Additionally, the data in the article refers to the average difference in life expectancy — of course, some men live longer than women in all countries.
The sex gap in life expectancy comes from gaps in death rates across age groups
The sex gap in life expectancy comes from sex differences in death rates across age groups — infants, youth, and older people.
Let’s look through them one at a time.
Infant death rates tend to be higher among boys than girls
The sex gap in life expectancy begins at birth, as newborn boys have a higher probability of death than newborn girls.
Boys are more likely to be born premature;2 and they also have higher death rates in the first week of life.3 This gap continues throughout infancy.
This is shown in the chart, where infant death rates in girls are shown on the horizontal axis, and death rates in boys are shown on the vertical axis.
In 2021, all countries are above the diagonal line, which shows that infant death rates were higher in boys.4
The sex gap in infant death rates is due to a range of factors.5
One key reason is that boys tend to be more vulnerable to infectious diseases, which may be due to a less developed immune system.6 Another is that boys are more susceptible to some genetic disorders due to having only one X chromosome.7
Youth death rates tend to be higher among men than women
After childhood, death rates rise due to accidents, violence, suicides, poisonings, and other ‘external causes of death’.8
These causes of death tend to be more common among men than women — which widens the sex gap in life expectancy.
The chart shows the gap in overall death rates at age 25, as an example — the gap in death rates is also seen at other ages.
As before, most countries are found above the diagonal line, which means death rates are higher among men.
Older age death rates tend to be higher among men than women
The sex gap in life expectancy is also sustained at older ages.
As people grow older, death rates rise steeply from a range of diseases, including respiratory and cardiovascular diseases, infections, cancers, and autoimmune diseases. Men tend to have higher prevalence rates and death rates from many chronic conditions, which further contributes to the gap in life expectancy.9
These differences are partly due to gender differences in health behaviors, such as smoking, alcohol, and drug use, and occupational risks, which tend to be more common in men and have growing consequences with age.10
As before, in 2021, all countries are above the diagonal line, which means death rates are higher in men than women.
The reasons for the sex gap in life expectancy have shifted over time
So far, we’ve seen that the death rate in males is higher among infants, young people, and older people.
But how much do these differences contribute to the overall gap in life expectancy? And how has this changed over time?
In a recent study by Virginia Zarulli et al. in 202111, the authors show how different age groups contribute to the gap.
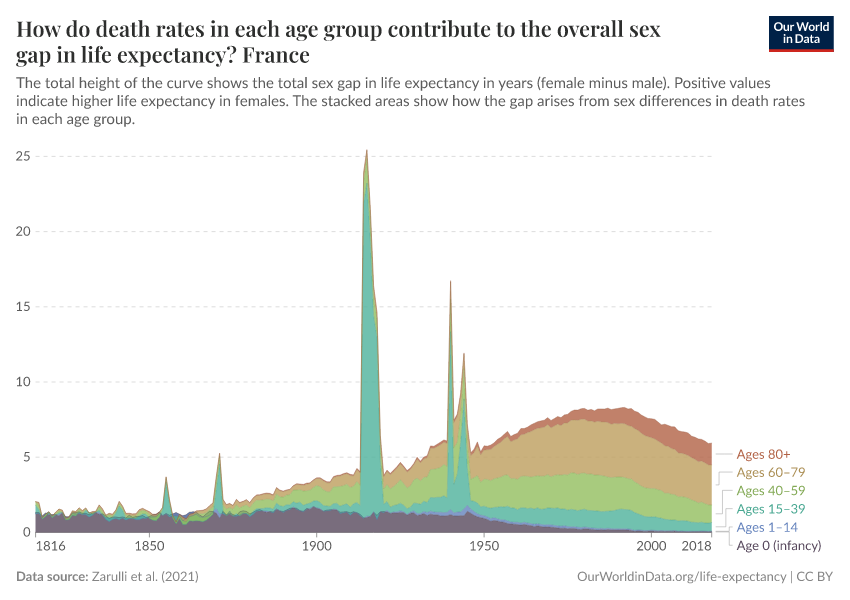
This is shown in the chart below for France, which has long-term mortality data.
The total sex gap in life expectancy is shown as the total height of the curve. The stacked areas show how the gap arises from sex differences in death rates in each age group.
You can see that both the overall sex gap in life expectancy and its composition have changed over time.
Before 1900, half of the gap was due to sex differences in infant mortality.
During the World Wars, the gap spiked due to a surge in death rates in young men.
However, over the 20th century, the gap also widened gradually. As the chart shows, this came from sex differences in mortality in youth and older age groups specifically.
Research suggests that the rise in smoking — which was especially prevalent among men — was a significant contributor to this widening gap.12 As smoking has fallen, the gap has narrowed.
You can see that the sources of the gap have shifted over time: most of the gap now comes from middle and older age death rates, with infant and child death rates making only a small contribution.
The chart below shows that there are also differences between countries. In Russia and Poland, for example, the overall sex gap in life expectancy is still large due to higher death rates in young and middle-aged men than women.
You can use the settings to explore this data for other countries.
Conclusion
The sex gap in life expectancy begins at birth: newborn boys have higher death rates than newborn girls, as they’re more vulnerable to diseases and genetic disorders.
It continues in youth, when boys have a higher death rate than girls, typically due to violence and accidents.
It’s sustained at older ages when men have higher death rates than women from chronic health conditions, which are partly due to higher rates of smoking, alcohol, and drug use.
As there are many reasons for the sex gap in life expectancy, its size varies between countries and has shifted over time.
In the past, gender differences in infant mortality were the leading cause of the gap in life expectancy. But now, differences at older ages are a larger contributor to the gap in life expectancy.
Acknowledgments
Edouard Mathieu, Max Roser, and Esteban Ortiz-Ospina provided valuable feedback that improved this article.
Endnotes
Until recently, in some countries such as India, Bangladesh, Pakistan, and Iran, male life expectancy was higher than female life expectancy.
Orzack, S. H., Stubblefield, J. W., Akmaev, V. R., Colls, P., Munné, S., Scholl, T., Steinsaltz, D., & Zuckerman, J. E. (2015). The human sex ratio from conception to birth. Proceedings of the National Academy of Sciences, 112(16). https://doi.org/10.1073/pnas.1416546112
Peelen, M. J. C. S., Kazemier, B. M., Ravelli, A. C. J., De Groot, C. J. M., Van Der Post, J. A. M., Mol, B. W. J., Hajenius, P. J., & Kok, M. (2016). Impact of fetal gender on the risk of preterm birth, a national cohort study. Acta Obstetricia et Gynecologica Scandinavica, 95(9), 1034–1041. https://doi.org/10.1111/aogs.12929
Zeitlin, J. (2002). Fetal sex and preterm birth: Are males at greater risk? Human Reproduction, 17(10), 2762–2768. https://doi.org/10.1093/humrep/17.10.2762
Boys are also more likely to be stillborn.
Mondal, D., Galloway, T. S., Bailey, T. C., & Mathews, F. (2014). Elevated risk of stillbirth in males: Systematic review and meta-analysis of more than 30 million births. BMC Medicine, 12(1), 220. https://doi.org/10.1186/s12916-014-0220-4
Carlsen, F., Grytten, J., & Eskild, A. (2013). Changes in fetal and neonatal mortality during 40 years by offspring sex: A national registry-based study in Norway. BMC Pregnancy and Childbirth, 13(1), 101. https://doi.org/10.1186/1471-2393-13-101
Fottrell, E., Osrin, D., Alcock, G., Azad, K., Bapat, U., Beard, J., Bondo, A., Colbourn, T., Das, S., King, C., Manandhar, D., Manandhar, S., Morrison, J., Mwansambo, C., Nair, N., Nambiar, B., Neuman, M., Phiri, T., Saville, N., … Prost, A. (2015). Cause-specific neonatal mortality: Analysis of 3772 neonatal deaths in Nepal, Bangladesh, Malawi and India. Archives of Disease in Childhood - Fetal and Neonatal Edition, 100(5), F439–F447. https://doi.org/10.1136/archdischild-2014-307636
In some countries, such as India, Bangladesh, Pakistan, and Iran, infant mortality was higher among females until recently.
Read more on our page on the gender ratio.
Drevenstedt, G. L., Crimmins, E. M., Vasunilashorn, S., & Finch, C. E. (2008). The rise and fall of excess male infant mortality. Proceedings of the National Academy of Sciences, 105(13), 5016–5021. https://doi.org/10.1073/pnas.0800221105
Guerra-Silveira, F., & Abad-Franch, F. (2013). Sex Bias in Infectious Disease Epidemiology: Patterns and Processes. PLoS ONE, 8(4), e62390. https://doi.org/10.1371/journal.pone.0062390 Conversely, females tend to have a higher vulnerability to autoimmune diseases.
Ji, J., Sundquist, J., & Sundquist, K. (2016). Gender-specific incidence of autoimmune diseases from national registers. Journal of Autoimmunity, 69, 102–106. https://doi.org/10.1016/j.jaut.2016.03.003
Libert, C., Dejager, L., & Pinheiro, I. (2010). The X chromosome in immune functions: When a chromosome makes the difference. Nature Reviews Immunology, 10(8), 594–604. https://doi.org/10.1038/nri2815
Schurz, H., Salie, M., Tromp, G., Hoal, E. G., Kinnear, C. J., & Möller, M. (2019). The X chromosome and sex-specific effects in infectious disease susceptibility. Human Genomics, 13(1), 2. https://doi.org/10.1186/s40246-018-0185-z
These external causes of death vary over time and between countries. They include occupational risks and traffic deaths. They have surged across countries during major conflicts like the two World Wars and have risen and fallen in some countries with the rise in automobile use.
Remund, A., Camarda, C. G., & Riffe, T. (2018). A Cause-of-Death Decomposition of Young Adult Excess Mortality. Demography, 55(3), 957–978. https://doi.org/10.1007/s13524-018-0680-9
Remund, A., Camarda, C. & Riffe, T. (2021). Is young adult excess mortality a natural phenomenon? Population & Societies, 590, 1-4. https://doi.org/10.3917/popsoc.590.0001 Available here.
Feraldi, A., & Zarulli, V. (2022). Patterns in age and cause of death contribution to the sex gap in life expectancy: A comparison among ten countries. Genus, 78(1), 23. https://doi.org/10.1186/s41118-022-00171-9
See Figure 3A and B:
Zazueta-Borboa, J.-D., Aburto, J. M., Permanyer, I., Zarulli, V., & Janssen, F. (2023). Contributions of age groups and causes of death to the sex gap in lifespan variation in Europe. Population Studies, 1–22. https://doi.org/10.1080/00324728.2023.2222723
Men also tend to have higher prevalence rates of heart disease, stroke, and diabetes. In comparison, women have higher rates of autoimmune diseases such as arthritis, anxiety, and depression — but these patterns are not seen in all countries.
For example, in Spain, Russia, and Korea, gender differences in the prevalence of heart disease are small or insignificant. In China, women are more likely than men to have heart disease.
Crimmins, E. M., Shim, H., Zhang, Y. S., & Kim, J. K. (2019). Differences between Men and Women in Mortality and the Health Dimensions of the Morbidity Process. Clinical Chemistry, 65(1), 135–145. https://doi.org/10.1373/clinchem.2018.288332
Jamal, A., Phillips, E., Gentzke, A. S., Homa, D. M., Babb, S. D., King, B. A., & Neff, L. J. (2018). Current Cigarette Smoking Among Adults—United States, 2016. MMWR. Morbidity and Mortality Weekly Report, 67(2), 53–59. https://doi.org/10.15585/mmwr.mm6702a1
Oza, S., Thun, M. J., Henley, S. J., Lopez, A. D., & Ezzati, M. (2011). How many deaths are attributable to smoking in the United States? Comparison of methods for estimating smoking-attributable mortality when smoking prevalence changes. Preventive Medicine, 52(6), 428–433. https://doi.org/10.1016/j.ypmed.2011.04.007
Zarulli, V., Kashnitsky, I., & Vaupel, J. W. (2021). Death rates at specific life stages mold the sex gap in life expectancy. Proceedings of the National Academy of Sciences, 118(20), e2010588118. https://doi.org/10.1073/pnas.2010588118
Janssen, F. (2020). Changing contribution of smoking to the sex differences in life expectancy in Europe, 1950–2014. European Journal of Epidemiology, 35(9), 835–841. https://doi.org/10.1007/s10654-020-00602-x
Luy, M., & Wegner-Siegmundt, C. (2015). The impact of smoking on gender differences in life expectancy: More heterogeneous than often stated. The European Journal of Public Health, 25(4), 706–710. https://doi.org/10.1093/eurpub/cku211
Cite this work
Our articles and data visualizations rely on work from many different people and organizations. When citing this article, please also cite the underlying data sources. This article can be cited as:
Saloni Dattani and Lucas Rodés-Guirao (2023) - “Why do women live longer than men?” Published online at OurWorldinData.org. Retrieved from: 'https://archive.ourworldindata.org/20260518-093348/why-do-women-live-longer-than-men.html' [Online Resource] (archived on May 18, 2026).BibTeX citation
@article{owid-why-do-women-live-longer-than-men,
author = {Saloni Dattani and Lucas Rodés-Guirao},
title = {Why do women live longer than men?},
journal = {Our World in Data},
year = {2023},
note = {https://archive.ourworldindata.org/20260518-093348/why-do-women-live-longer-than-men.html}
}Reuse this work freely
All visualizations, data, and articles produced by Our World in Data are completely open access under the Creative Commons BY license. You have the permission to use, distribute, and reproduce these in any medium, provided the source and authors are credited.
The data produced by third parties and made available by Our World in Data is subject to the license terms from the original third-party authors. We will always indicate the original source of the data in our documentation, so you should always check the license of any such third-party data before use and redistribution.
All of our charts can be embedded in any site.