More than half a million children die from diarrhea each year. How do we prevent this?
Despite being treatable and preventable, 1.6 million people died from diarrheal diseases in 2017; one-third were children under five years old. This makes it one of the largest killers of children. Here we look at where and why children are dying from diarrheal diseases, and what we can do to stop this.
Diarrheal diseases are one of the biggest killers of children worldwide
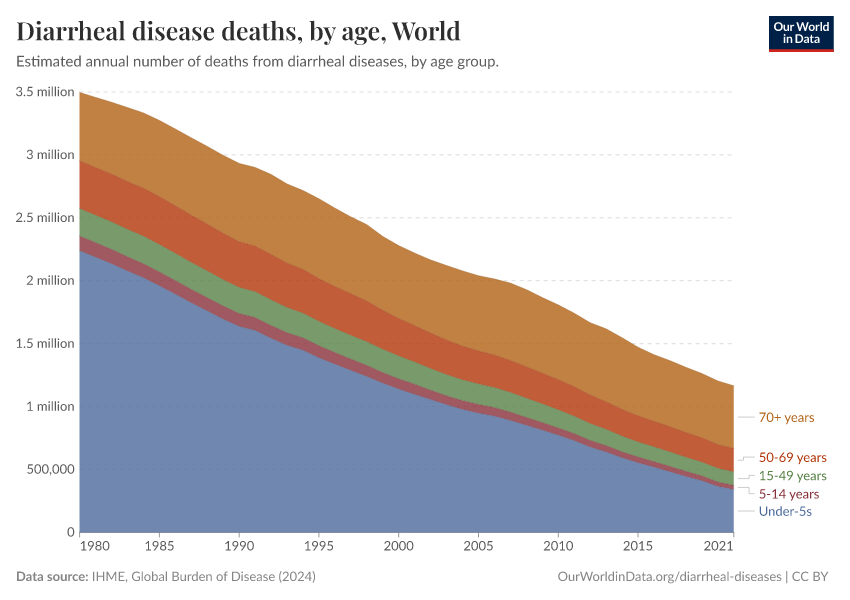
In 2017, almost 1.6 million people died from diarrheal diseases globally.
This is more than all deaths from all 'intentional injuries' combined in the same year: almost 800,000 died from suicide, 405,000 from homicide, 130,000 in conflict, and 26,500 from terrorism – in total 1,355,000.1
As the visualization shows, one-third of all who died from diarrheal diseases were children under five years old. For most of the past three decades under-5s have accounted for the majority of deaths from diarrheal diseases – back in 1990 it killed 1.7 million children.
Diarrheal disease was the cause of every tenth child's death in 2017 – more than half a million of the 5.4 million children that died in 2017 died from diarrheal disease.
Diarrheal diseases are the third leading cause of child mortality globally, falling just behind pneumonia and preterm birth complications.
Where are children dying from diarrheal diseases?
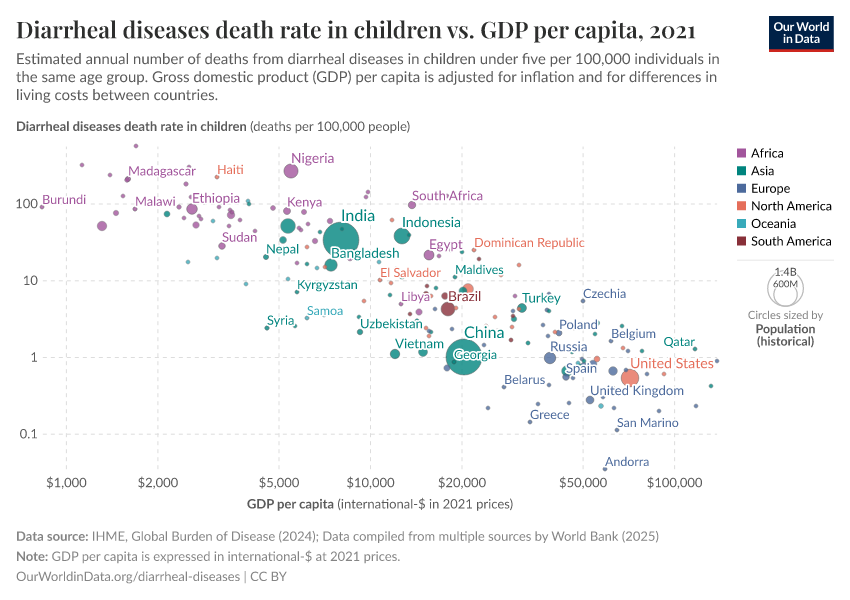
The death rate from diarrheal diseases is highest in the world's poorest countries: this chart shows the relationship between the death rate from diarrheal diseases and the country’s average income.
The death rate from diarrheal diseases in many of the poorest countries is higher than 100 annual deaths per 100,000 children. In those countries with the worst health – including Madagascar, Chad and the Central African Republic – the rate is higher than 300 per 100,000.
In high-income countries the death rate is very low. In many European countries, but also some rich Asian countries the rate is below 1 per 100,000 per year.
At lower levels of income risk factors for diarrheal diseases such as lack of access to clean water, rotavirus vaccine availability, undernutrition, stunting and others are the most prevalent.2
What causes diarrheal diseases in children?
Understanding the cause of disease is important so that we can set our priorities on the interventions and treatments that would save most lives, e.g. developing vaccines against the main agents for diarrhea and using antibiotic treatments only when they are appropriate.
Diarrheal diseases are caused primarily by viral and bacterial pathogens. The visualization shows the major pathogens responsible for diarrhea in children; the area of each box corresponds to the number of deaths from diarrhea in 2016 that can be attributed to each pathogen.
While bacterial pathogens (shown in red) are the major group of organisms responsible for diarrheal diseases, rotavirus is the single largest causative agent.3
Why are children still dying from diarrhea?
There are two main reasons why the number of children dying from diarrhea is still so large – the prevalence of diarrhea-associated risk factors and the lack of access to essential treatment.
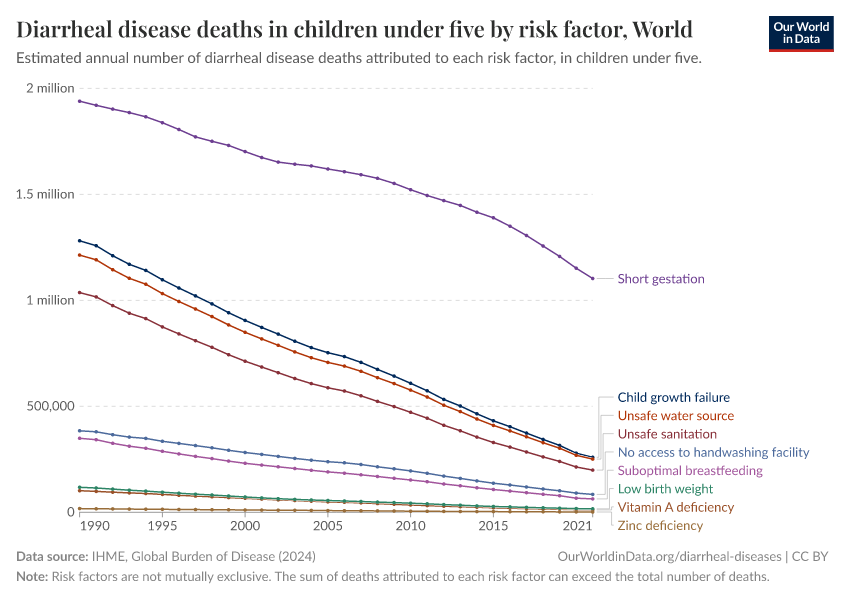
The figure shows the number of deaths associated with the major risks factors for diarrheal diseases: unsafe drinking water, poor sanitation and malnutrition are responsible for the largest portion of deaths.
Since 1990 we have made a lot of progress in reducing these major risks; you can read more in our research entries on Hunger and Undernourishment, Extreme Poverty and Water Use and Sanitation. But continued progress is still needed.
In addition to reducing exposure to risks factors, increasing access to oral rehydration therapy (ORT), therapeutic zinc use and the coverage of rotavirus vaccines were all shown to be essential for reducing the burden of diarrheal diseases in children.4
How can we stop child deaths from diarrhea?
Diarrheal diseases are both 'preventable and treatable', as the WHO says, because we already know how to deal with many of the risk factors that may lead to diarrhea and, if diarrhea cannot be avoided, we know how to treat it.
The table below lists the range of interventions available for the treatment of diarrhea we have today.5
Intervention | Estimate of the effect size |
|---|---|
Handwashing with soap | 48% risk reduction |
Improved water quality | 17% risk reduction |
Excreta disposal (improved sanitation) | 36% risk reduction |
Breastfeeding education | 43% increase in exclusive breastfeeding rates at day 1, 30% increase until 1 month, and 90% increase from 1-6 months |
Preventive zinc supplementation | 13% reduction in diarrhea incidence, but no effect on mortality |
Therapeutic zinc supplementation | 46% reduction in all-cause mortality and 23% reduction in hospitalization due to diarrhea |
Rotavirus vaccines | 74% effectiveness against very severe rotavirus infection; 61% against severe; 47% reduction in hospitalization |
Cholera vaccines | 52% effective against cholera infection |
Oral rehydration solution (ORS) | 69% reduction in diarrhea-specific mortality |
Dietary management for diarrhea | 47% reduction in diarrhea treatment failure and 47% reduction in treatment failure |
Antibiotics for cholera | 63% reduction in clinical failure rates |
Antibiotics for Shigella | 82% reduction in clinical failure rates |
Antibiotics for cryptosporidiosis | 52% reduction in clinical failure rates |
Community-based interventions (home visits and healthcare promotion) | 160% increase in ORS use and 80% increase in zinc use. 9% increase in seeking care for diarrhea and 75% reduction in inappropriate antibiotic use |
Some of these interventions, such as ORS, breastfeeding and improvements in sanitation broadly target all-causes of diarrhea, whereas vaccination and antibiotic use are specifically directed against the causative agents of the disease.
Water, sanitation and hygiene (WASH) interventions are the best way to prevent diarrheal diseases. Hand washing with soap, better water quality and better sanitation have been shown to reduce the risk of diarrheal infections by 47%, 17% and 36%, respectively.6
Educating mothers about the importance of breastfeeding is also important. Breastfeeding allows for the transfer of maternal immunity to the child – in developing countries infants that are not breastfed are six times more likely to die from infectious diseases, such as those causing to diarrhea, in the first 2 months of their lives.7
Another way to prevent diarrheal diseases is vaccination. Until relatively recently, there were few vaccines available to prevent diarrheal diseases. Cholera vaccine has been licensed since 1991 but it is primarily given to travelers and used as an outbreak control measure. This is because targeted immunization combined with other sanitary measures is more cost-effective than immunizing every individual with a vaccine that only provides a few years of protection.8
In 2006, however, new vaccines against rotavirus – the leading cause of childhood diarrhea as the treemap above shows – have been introduced. The most recent studies show that, while the effectiveness of the new rotavirus vaccines vary across different countries, it works well in protecting children against rotavirus disease.9
When preventative measures fail, several options for the treatment of diarrheal diseases are available, including nutritional interventions and antibiotic use when necessary. But the single best treatment for diarrheal diseases is a surprisingly simple mixture of water, salt and sugar: otherwise known as the oral rehydration solution.10
The estimates of ORS effectiveness vary by source, with some suggesting that the current use of ORS helps to prevent 69% of diarrheal deaths and, if its coverage would be increased close to 100%, 93% of diarrheal deaths could be prevented.11
Endnotes
The data can be seen here. The precise numbers are 793,823+405,346+26,445+129,720=1,355,334
Troeger, Christopher, et al. "Estimates of the global, regional, and national morbidity, mortality, and aetiologies of diarrhoea in 195 countries: a systematic analysis for the Global Burden of Disease Study 2016."The Lancet Infectious Diseases 18.11 (2018): 1211-1228.
The previous version of the treemap incorrectly classified Cryptosporidium as a bacterial pathogen. It should in fact be grouped with protist. Thank you to the readers who noticed the mistake.
Troeger, C., Blacker, B. F., Khalil, I. A., Rao, P. C., Cao, S., Zimsen, S. R., … & Alvis-Guzman, N. (2018). Estimates of the global, regional, and national morbidity, mortality, and aetiologies of diarrhoea in 195 countries: a systematic analysis for the Global Burden of Disease Study 2016. The Lancet Infectious Diseases, 18(11), 1211-1228.
Das, J. K., Salam, R. A., & Bhutta, Z. A. (2014). Global burden of childhood diarrhea and interventions.Current Opinion in Infectious Diseases, 27(5), 451-458.
Cairncross, S., Hunt, C., Boisson, S., Bostoen, K., Curtis, V., Fung, I. C., & Schmidt, W. P. (2010). Water, sanitation and hygiene for the prevention of diarrhoea. International Journal of Epidemiology, 39(suppl_1), i193-i205.
Victoria, C. G. (2000). Effect of breastfeeding on infant and child mortality due to infectious diseases in less developed countries: a pooled analysis. Lancet (British edition), 355(9202), 451-455.
Apps.who.int. (2019). Weekly Epidemiological Record. [online] Available at: https://apps.who.int/iris/bitstream/handle/10665/258763/WER9234.pdf?sequence=1 [Accessed 12 Aug. 2019].
Sinclair, David, et al. "Oral vaccines for preventing cholera."Cochrane Database of Systematic Reviews 3 (2011).
Jonesteller, Christine L., et al. "Effectiveness of rotavirus vaccination: a systematic review of the first decade of global postlicensure data, 2006–2016."Clinical Infectious Diseases 65.5 (2017): 840-850.
Aliabadi, Negar, et al. "Global impact of rotavirus vaccine introduction on rotavirus hospitalisations among children under 5 years of age, 2008–16: findings from the Global Rotavirus Surveillance Network."The Lancet Global Health 7.7 (2019): e893-e903.
Fontaine, Olivier, Paul Garner, and M. K. Bhan. "Oral rehydration therapy: the simple solution for saving lives."BMJ,334.suppl 1 (2007): s14-s14.
Munos, M. K., Walker, C. L. F., & Black, R. E. (2010). The effect of oral rehydration solution and recommended home fluids on diarrhoea mortality. International Journal of Epidemiology, 39(suppl_1), i75-i87.
Cite this work
Our articles and data visualizations rely on work from many different people and organizations. When citing this article, please also cite the underlying data sources. This article can be cited as:
Bernadeta Dadonaite (2019) - “More than half a million children die from diarrhea each year. How do we prevent this?” Published online at OurWorldinData.org. Retrieved from: 'https://archive.ourworldindata.org/20260518-095641/childhood-diarrheal-diseases.html' [Online Resource] (archived on May 18, 2026).BibTeX citation
@article{owid-childhood-diarrheal-diseases,
author = {Bernadeta Dadonaite},
title = {More than half a million children die from diarrhea each year. How do we prevent this?},
journal = {Our World in Data},
year = {2019},
note = {https://archive.ourworldindata.org/20260518-095641/childhood-diarrheal-diseases.html}
}Reuse this work freely
All visualizations, data, and articles produced by Our World in Data are completely open access under the Creative Commons BY license. You have the permission to use, distribute, and reproduce these in any medium, provided the source and authors are credited.
The data produced by third parties and made available by Our World in Data is subject to the license terms from the original third-party authors. We will always indicate the original source of the data in our documentation, so you should always check the license of any such third-party data before use and redistribution.
All of our charts can be embedded in any site.